Anorectal Dyssynergia
Anorectal Dyssynergia is a functional bowel disorder that affects the normal coordination of muscles involved in bowel movements. In this condition, the muscles of the rectum and anal sphincter do not work together properly, making it difficult to pass stool effectively. As a result, individuals may experience chronic constipation and difficulty during bowel movements.
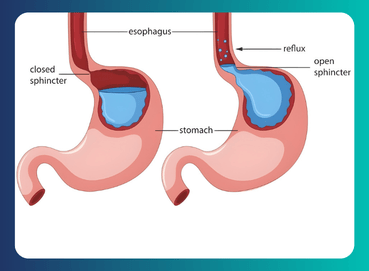
Normally, when a person tries to pass stool, the pelvic floor muscles relax while the rectal muscles push the stool out. In anorectal dyssynergia, these muscles may contract instead of relaxing, which disrupts the normal process of defecation.
Common Symptoms of Anorectal Dyssynergia
People with anorectal dyssynergia may experience the following symptoms:
Chronic Constipation
Persistent constipation that does not improve with normal dietary or lifestyle changes.
Excessive Straining
Excessive effort or straining during bowel movements.
Incomplete Bowel Evacuation
A persistent feeling that the bowel movement was not fully completed.
Difficulty Passing Stool
Difficulty coordinating muscles needed to pass stool effectively.
Hard or Infrequent Stools
Passing hard stools or having fewer bowel movements than normal.
Manual Assistance
Some individuals may need manual assistance to help pass stool.
Abdominal Discomfort
Discomfort, pressure, or bloating in the abdomen due to bowel issues.
Causes and Risk Factors of Anorectal Dyssynergia
Anorectal dyssynergia occurs when there is poor coordination between the pelvic floor muscles and the anal sphincter during bowel movements. This lack of coordination can make it difficult to pass stool and may lead to chronic constipation and discomfort.
- Pelvic floor muscle dysfunction
- Poor coordination of rectal and anal muscles
- Chronic constipation
- Nerve damage affecting bowel function
- Long-term straining during bowel movements
- Behavioral or functional bowel disorders
Diagnosis of Anorectal Dyssynergia
Doctors may use several tests to diagnose anorectal dyssynergia and evaluate how well the pelvic floor muscles function during bowel movements.
-
Anorectal Manometry
This test measures the pressure and coordination of the rectal and anal muscles to determine how well they function during bowel movements.
-
Balloon Expulsion Test
A small balloon is placed in the rectum and the patient is asked to expel it. Difficulty expelling the balloon may indicate pelvic floor dysfunction.
-
Defecography
This imaging test evaluates the process of bowel movement and helps identify abnormalities in the rectum and pelvic floor muscles.
-
Colonoscopy
A colonoscopy may be performed to rule out structural problems or other conditions affecting the colon and rectum.
-
Pelvic Floor Physical Examination
Doctors may perform a physical examination to assess the coordination and strength of the pelvic floor muscles.
Lifestyle Tips for Better Bowel Health
Adopting healthy lifestyle habits can help improve bowel function and manage symptoms related to anorectal dyssynergia. Proper diet, hydration, and healthy bowel habits play an important role in maintaining digestive health.
- Eat a fiber-rich diet
- Drink plenty of water
- Maintain regular bowel habits
- Exercise regularly
- Avoid excessive straining during bowel movements
- Follow proper toilet posture
Treatment Options for Anorectal Dyssynergia
Treatment focuses on improving the coordination of pelvic floor muscles and relieving symptoms such as chronic constipation and difficulty passing stool.
Frequently Asked Questions
Find answers to common questions about anorectal dyssynergia, including its symptoms, causes, diagnosis, and treatment options.
Anorectal dyssynergia is a condition where the pelvic floor muscles and anal sphincter do not coordinate properly during bowel movements, making it difficult to pass stool.
Common symptoms include chronic constipation, excessive straining during bowel movements, difficulty passing stool, and a feeling of incomplete bowel evacuation.
This condition can be caused by pelvic floor muscle dysfunction, poor coordination between rectal and anal muscles, nerve damage, or long-term straining during bowel movements.
Treatment usually includes biofeedback therapy, pelvic floor physical therapy, dietary changes to increase fiber intake, medications for constipation relief, and lifestyle modifications.