Gastroparesis
Gastroparesis is a digestive disorder in which the stomach takes longer than normal to empty its contents into the small intestine. This condition occurs when the muscles of the stomach do not function properly, slowing down the movement of food through the digestive tract.
Normally, the stomach contracts to push food into the small intestine for digestion. In gastroparesis, these contractions become weak or irregular, causing delayed stomach emptying. This can lead to symptoms such as nausea, vomiting, bloating, and a feeling of fullness after eating small amounts of food.
Common Symptoms of Gastroparesis
People with gastroparesis may experience the following symptoms:
Nausea and Vomiting
Frequent nausea and vomiting caused by delayed stomach emptying.
Feeling Full Quickly
Feeling full soon after starting a meal, even when eating small portions.
Bloating and Abdominal Discomfort
Bloating or discomfort in the stomach due to slow digestion.
Loss of Appetite
Reduced appetite caused by prolonged stomach fullness.
Unexplained Weight Loss
Weight loss due to reduced food intake and poor digestion.
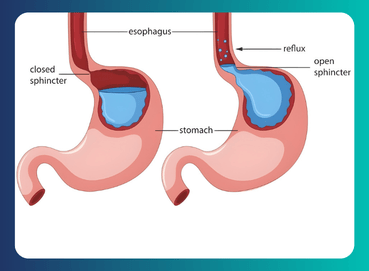
Acid Reflux or Heartburn
Acid reflux or heartburn due to delayed stomach emptying.
Poor Blood Sugar Control
Difficulty managing blood sugar levels in diabetic patients.
Persistent Indigestion
Continuous indigestion or discomfort after meals.
Causes of Gastroparesis
Gastroparesis occurs when the stomach muscles do not function properly, causing delayed emptying of food from the stomach. This condition is often related to damage to the nerves that control stomach movement, especially the vagus nerve. When these nerves are affected, the normal digestive process slows down and leads to various digestive symptoms.
- Diabetes
- Nerve damage affecting stomach muscles
- Certain medications that slow digestion
- Previous stomach surgery
- Viral infections
- Neurological disorders
- Autoimmune conditions
Diagnosis of Gastroparesis
Doctors may recommend several diagnostic tests to evaluate stomach emptying and confirm the presence of gastroparesis.
-
Gastric Emptying Study
This is the most common test used to diagnose gastroparesis. During the test, the patient eats a small meal containing a safe radioactive substance, and imaging is used to measure how quickly food leaves the stomach.
-
Upper GI Endoscopy
An upper gastrointestinal endoscopy allows doctors to examine the stomach and upper digestive tract using a thin flexible tube with a camera to rule out blockages or other abnormalities.
-
Ultrasound or CT Scan
Imaging tests such as ultrasound or CT scans help doctors check for structural problems in the stomach or surrounding organs that may cause digestive symptoms.
-
Blood Tests
Blood tests may be performed to detect infections, nutritional deficiencies, or blood sugar levels, especially in patients with diabetes.
-
Barium Swallow Study
In this imaging test, the patient drinks a barium-containing liquid that coats the digestive tract, allowing doctors to observe the movement of food through the stomach using X-ray imaging.
Dietary and Lifestyle Tips for Gastroparesis
Making certain dietary and lifestyle adjustments can help manage the symptoms of gastroparesis and improve digestion. Proper eating habits and food choices can support better stomach emptying and reduce discomfort after meals.
- Eat small and frequent meals
- Choose soft and easily digestible foods
- Avoid high-fat and high-fiber foods
- Chew food thoroughly before swallowing
- Stay upright after meals
- Drink adequate fluids
Treatment Options for Gastroparesis
Treatment focuses on improving stomach motility and relieving symptoms caused by delayed stomach emptying.
Frequently Asked Questions
Find answers to common questions about gastroparesis, including its symptoms, causes, diagnosis, and treatment options.
Gastroparesis is a digestive disorder in which the stomach takes longer than normal to empty food into the small intestine. It occurs when the stomach muscles do not function properly, often due to nerve damage.
Common symptoms include nausea, vomiting, bloating, early fullness after eating, loss of appetite, acid reflux, and unexplained weight loss. Some patients may also experience persistent indigestion.
Gastroparesis is often caused by damage to the vagus nerve that controls stomach muscles. Common causes include diabetes, previous stomach surgery, certain medications, viral infections, and neurological disorders.
Treatment may include medications to stimulate stomach muscles, anti-nausea drugs, dietary changes such as eating small frequent meals, and controlling blood sugar levels in diabetic patients. In severe cases, endoscopic or surgical procedures may be recommended.